“One in three adults over 65 will fall each year… but the groundwork starts much earlier.”
Did you know that one in three adults over 65 fall each year? When I heard this statistic I was horrified.
But I shouldn’t have been surprised because of what had happened in my own family. My father had a fall when he was 81, he never walked again and spent his last 3.5 years bed bound.
My mother fell last year and was slightly “luckier,” they were able to operate to replace her hip and add some screws to fixate broken bones. I have seen how much it has slowed her down and caused her so much pain.
My parents are two classic examples of outcomes from falling in older age, you could:
- fracture a hip and need surgery,
- hit your head and have brain damage or even die,
- onset of dementia,
- become bed bound for the rest of your days.
So the stakes are high!
But it doesn’t have to be this way, there are many things that you can do in your 50s and 60s to give you the best chance of not falling over in your 70s and 80s.
This article will focus on positive, preventative steps towards falls prevention. I will give you 12 steps that you can take to prevent yourself from falling, and I’ll back it up with solid evidence!
Why Falls Prevention Should Start in Your 50s (Not Your 70s)
Muscle Loss (Sarcopenia) Begins Earlier Than You Think
- Age-related muscle decline – as you age your muscles lose size and strength. It becomes naturally a lot harder to build on or even maintain the strength that you had before.
- Calf and ankle strength importance – research has found that this is one of the best indicators of your likelihood of having a fall.
Balance Quietly Declines
- Reduced proprioception (proprioception is the feedback from your body to your brain as to where you are spatially).
- Slower reflexes – along with reduced proprioception, slower reflexes makes it harder for you to make corrections when you are walking. You know how you might trip on something on the ground, but your body is quick enough to make corrections to ensure that you don’t fall? well your body becomes much less likely to do this as you age.
Vision and Reaction Time Change
- Reduced vision = greater injury risk. If you can’t see things around you very well, you are much more likely to have a fall because of your environment. It might be that last step on the stairs that you miss, or a small raise in the pavement.

The 7 Biggest Risk Factors for Falls Later in Life
- Weak calf muscles
- Poor ankle mobility
- Foot pain (heel pain, arthritis, neuropathy)
- Unsafe footwear
- Sedentary lifestyle
- Poor lighting/home hazards
- Medications causing dizziness
Strength Training: Your #1 Falls Prevention Tool
Strength training has been quoted in different systematic reviews to reduce your chance of falling by between 19% and 38%. Personally I’ll take any reduction in the chance of falling!
Visser, O’Neill and Losier et. al. did a study across 500 people to find what the normative (average) number of calf raises people can perform at different ages and found the following:

To find out if you are at least average or even better, see how many times you can fully raise one heel and bring it down again. You can hold something for balance, but don’t use it to assist your lift.
Focus on the Lower Legs
The Calf Muscle Is Critical
The calf muscle is crucial to preventing falls for a number of reasons including:
- The calf is the pump that takes used blood back to the heart to get re-oxygenated by the lungs. As we age the valves in our veins start to fail and this makes the calf muscle’s role all the more important. To read more about the calf muscle pump concept see my previous post here.
- Push-off strength prevents stumbles – the better we are able to push off, the less likely we are to fall. The calf muscle plantar-flexes the foot to propel us forward. So the strength of the calf muscles is again so important.
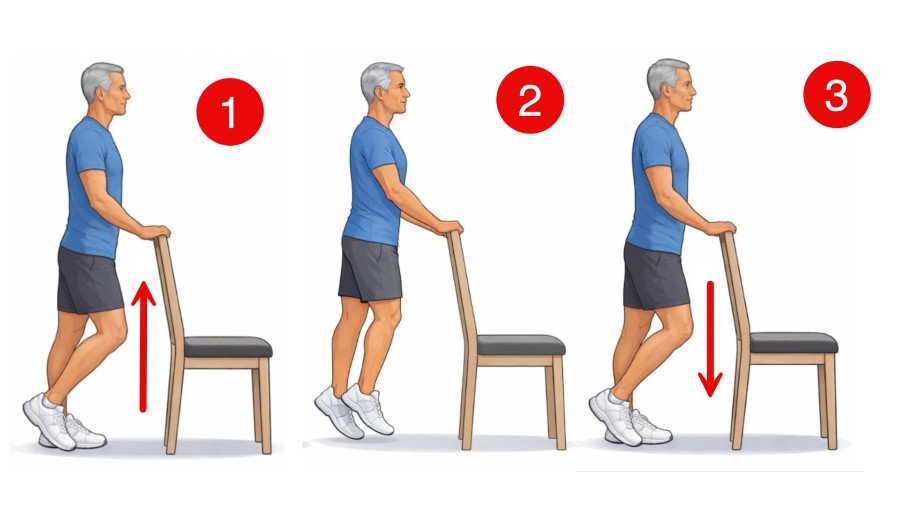
Calf raises:
See the diagram below.
Use a chair to keep yourself safe but don’t use it to lift you up.
Stand on one leg and fully lift the heel of the foot on the floor off the floor.
Go slowly up and down counting as you go, then do the other leg.
See how many you can comfortably do, and build up your tolerance by consistently doing these exercises every two or three days.
Toe raises:
in the 2 videos below are a quick demonstration of two exercises: the big toe raise and the lesser toe raise.
Both are iportant and short be done 3 times per week.
Do each exercise for around a minute.
TIP: this can be difficult to isolate the toes, the best way to start is to imagine that you are lifting just the big toe, after a while your brain will make the connection. Try it!
Frequency and Progression
As a group of exercises they should be performed 2-3 times per week.
Progressively increase the number you do as you become more capable. This is crucial to continue reducing your risk of a fall.
The key is to be consistent.
If you’re anything like me you’re likely to go really hard for the first couple of weeks, which is hard to maintain, so you end up stopping altogether. Don’t do this, don’t be like Matt!
Build up slowly and consistently and you will be a much lower chance of having a fall as you get older.
Balance Training: Train It Before You Lose It
Single-Leg Stance
- 10–30 seconds per side. Hold onto a chair or the kitchen bench and stand on one leg. Try to hold it for up to 30 seconds on each leg. The more consistent you are with this exercise, the better you will become at it.
Heel to Toe Drill:
This one can be done on any type of flooring.
Place your lead foot so that the heel is almost touching the big toe of then hind foot.
Bring your hind foot around until its heel is almost touching the big toe of the other foot and so on.
To help balance you can put your arms out like a tight-rope walker.
Dynamic Balance
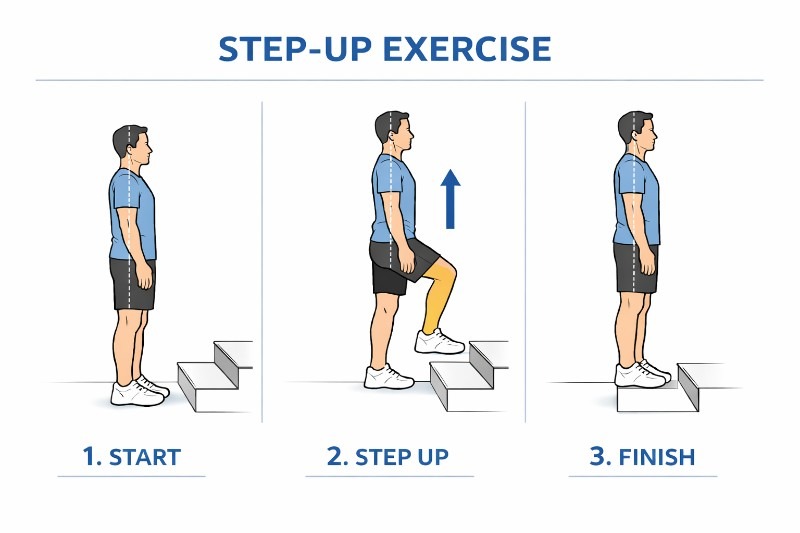
Step-ups
- this is a simple exercise where you can use the bottom stair of a staircase.
- step with one foot onto the step trying to keep your body nice and straight.
staying straight is a key to better balance, so if you find that you are leaning in one direction, then practice 3-4 times per week to increase your strength. - don’t forget to do these on the left and the right.
- See the diagram below (try to ignore the weird step in Step 3)!
Side stepping – see the diagram below. A simple exercise where you walk sideways in one direction, and then back in the other direction.
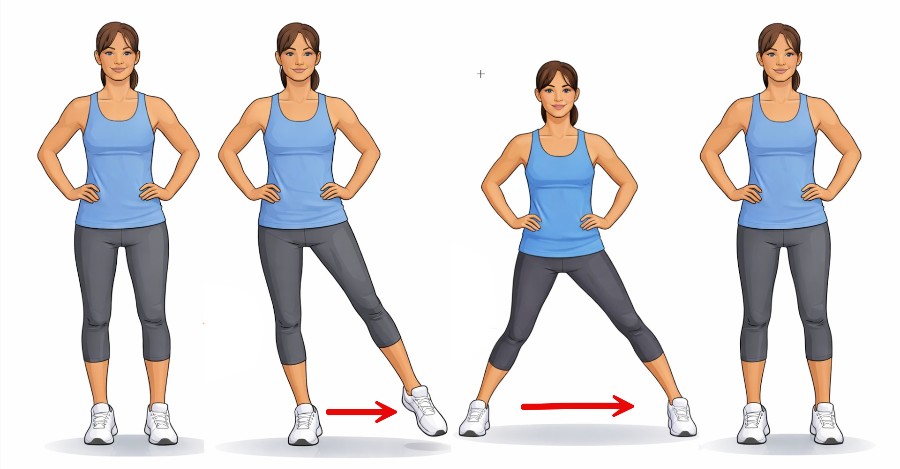
Balance is a skill. Skills decline if unused.
Ankle Mobility: The Hidden Factor in Falls Prevention
Most people only stretch the gastrocnemius muscle when they do calf stretches.
It is important to also stretch the soleus muscle, which will only be stretched by bending the back knee.
See the diagrams below for correct technique
How Many?
- hold each position for 20 seconds
- do 3 repetitions on each side
- twice daily.
Gastrocnemius stretch

Soleus Stretch

Gastrocnemius Stretch: The back leg knee remains straight and the heel remains on the floor.
Soleus Stretch: The back leg is slightly bent and the heel remains on the floor. You should feel this stretch in the lower portion of your calf.
Foot Health Matters More Than You Think
Treat Foot Pain Early
- Plantar fasciitis – a pain that occurs in the bottom of the heel, most commonly on the first steps of the day or after having a rest and getting up again. This condition can be very effectively treated by your podiatrist.
Don’t wait for it to become a chronic problem before you seek help.
To read more about plantar fasciitis and heel pain in general see my earlier post here. - Arthritis – most of us will get some form of this if we live long enough. Some people will get more aggressive types like rheumatoid and psoriatic earlier in life. Combine with your doctor, physiotherapist and podiatrist toi manage this condition and minimise your pain.
Arthritis can be a major factor in falls, I know my father had terrible arthritis in his hips, knees and feet and this made him so much more prone to having a fall, which he did.
You can also find out more about arthritis in my earlier blog post here.
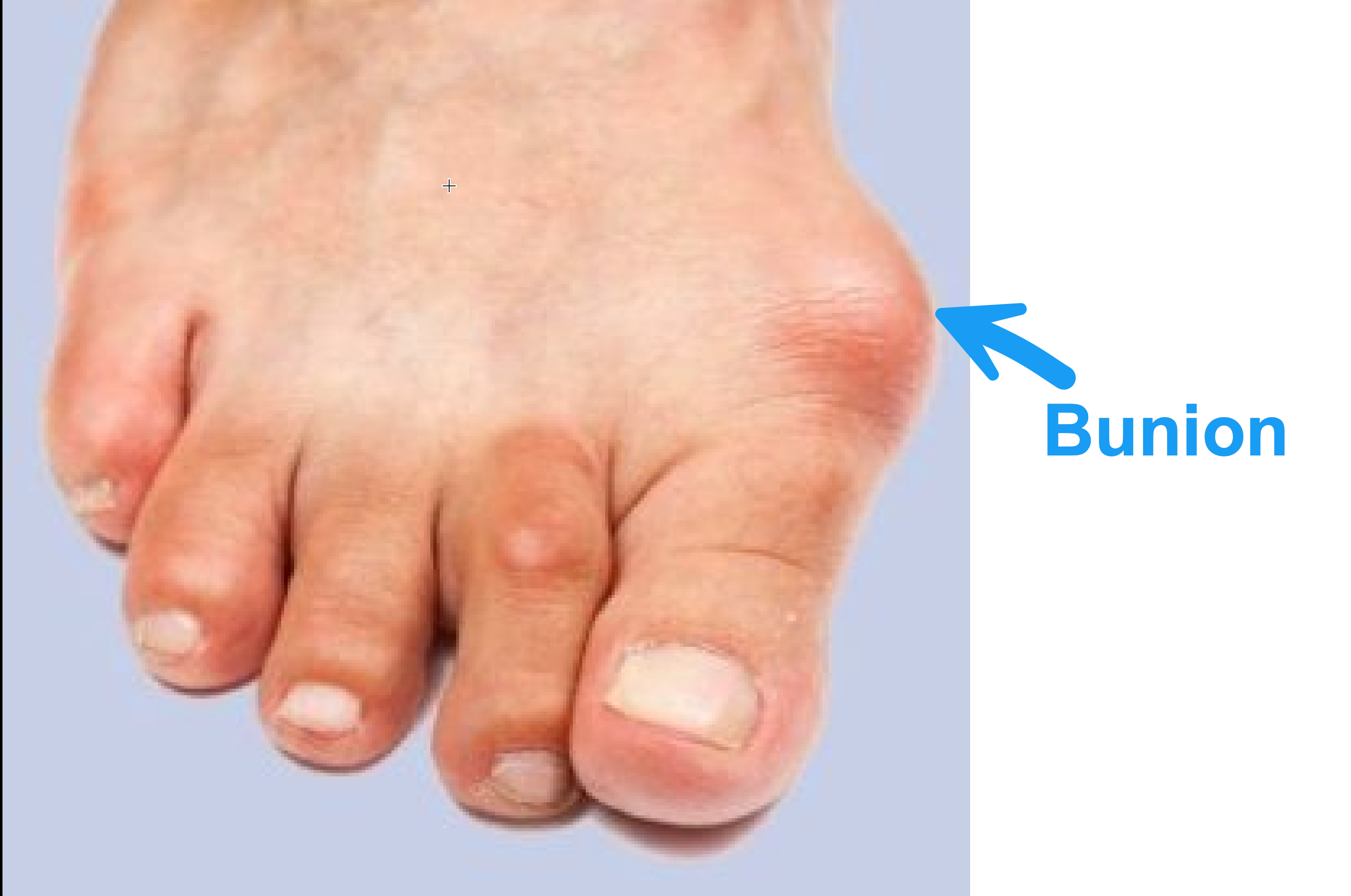
- Bunions – the earlier you get only there the better. I’ve often heard people call corns or warts bunions. Bunions are a deviation of the big toe which makes your feet wider and less efficient.
- Take a look at the image to the right.
If you’d like to learn more about bunions click here for my article on bunions and hammer toes.
Sensory Changes Can Have Dramatic Effects
Sensory changes can occur for any of the following reasons:
- Diabetes (type 1 or 2),
- Chemotherapy,
- Age (risk rises after reaching 50 years old),
- Lack of Vitamin B12
- Alcoholism,
- Malnutrition,
- High levels of Vitamin B6 (recent research has found that many common multivitamins have higher than recommended levels of Vitamin B6),
- Idiopathic (when none of the above are present with neuropathy, we call it idiopathic) we’re the idiots, not you!
Why Peripheral Neuropathy is Dangerous
Althoughwe don’t realise it, our feet are constantly feeding back information to our brains about how steady the surface we’re walking on is, and our eyes are telling us about what’s coming up.
Our brain then tells the muscles in our legs and feet when to fire and how much force to exert.
Do you remember when you were younger and you would take a misstep or slightly roll your ankle? In most young people your brain and your muscles will quickly re-adjust to make sure that you don’t fall over.
Peripheral neuropathy removes that feedback from the feet to the brain, meaning that instead of correcting when we take a misstep, we just keep going in that direction until we hit something that stops us – usually the ground or floor.
To find out more about peripheral neuropathy you can find my article by clicking here.
Don’t Ignore Nail and Skin Issues
- Thick nails affect balance
- Corns change gait
The Right Footwear Can Reduce Falls Risk
Look For:
- Firm heel counter
- Non-slip sole
- Low heel
- Wide toe box
- Secure fastening
Avoid:
- Slippers
- Backless shoes
- Worn tread
- High heels
Home Modifications That Prevent Falls
- Remove loose rugs
- Improve lighting
- Handrails on stairs
- Grab rails in bathroom
- Night lights
Cardiovascular Fitness and Circulation
- Walking regularly
- Why reduced circulation can impair stability
- The calf pump and venous return
Fear of Falling — The Psychological Factor
Unfortunately after your first fall it is easy to get stuck in a vicious cycle as below:
- After one fall, activity decreases, this leads to
- Muscle loss accelerating, which can lead to
- Confidence dropping which can make you less resilient and more likely yo have another fall.
The earlier you start on strengthening and stretching, the more likely you are to get caught up in this cycle in the first place.
When to See a Professional
- Recurrent falls
- Dizziness
- Foot numbness
- Sudden weakness
- New medications
Professionals who can help you are:
- GP
- Podiatrist
- Physiotherapist
A Simple Weekly Falls Prevention Plan (Action Section)
Example Week:
Monday: Strength (20 min)
Wednesday: Balance drills (10 min)
Friday: Strength + mobility
Daily: Walk 20–30 mins
Conclusion
Remember:
Falls prevention isn’t about wrapping yourself in cotton wool.
It’s about staying strong, mobile and independent.
Don’t say “One day,” say “Day One!”
Frequently Asked Questions (FAQs)
- Q. What is falls prevention?
A. Falls prevention is being aware of the risks of having a fall that relate to you and taking every step possible to preventing a fall. - Q. At what age should falls prevention begin?
A. Whatever age you are right now is the best time to start!
Ideally it should start in your 20s by living a healthy life and especially maintaining a healthy weight. But starting in your 50s, 60s or 70s is much better than never starting at all. - Q.Can exercise really prevent falls?
A. 100% and absolutely! A combination of cardiovascular exercise and weight training equips your muscles to be able to prevent a fall in the first place.
As a bonus it strengthen your bones so that if you do fall you are less likely of it being catastrophic. - Q. What shoes are best for falls prevention?
A. Shoes that are best for avoiding falls usually have the following features:
– heel cup at the back or at least a heel strap
– have a non-slip rubber sole,
– are not too long or too bulky,
– are nice and light,
– Have a heel of around 1.5 to 2cm (high heels can significantly increase your risk of a fall),
– be properly fitted to your feet.
- Q. What is falls prevention?